Telemedicine is the practice of using telecommunications and information technology to provide remote healthcare services. It enables healthcare professionals to evaluate, diagnose, treat, and monitor patients without an in-person visit.
The scope of telemedicine is broad, encompassing various forms, including live video consultations (virtual visits), “store-and-forward” technologies for sharing medical data like X-rays and lab results, and remote patient monitoring (RPM) using devices like continuous glucose monitors.
By leveraging digital tools, telemedicine improves access to care, enhances patient convenience, and increases the efficiency of healthcare delivery, especially for those in rural or underserved areas.
The Pandemic-Accelerated Mainstream Adoption
While telemedicine was on a steady growth trajectory, its adoption was dramatically accelerated by the COVID-19 pandemic. The need for social distancing and the overwhelmed healthcare system made virtual care a necessity rather than an alternative. This period saw a massive expansion of services, a relaxation of regulatory barriers, and unprecedented patient and provider acceptance, solidifying telemedicine’s place as a mainstream component of modern healthcare.
Three Modalities of Telemedicine
Based on standard industry practices, the three primary modalities of telemedicine are:
Synchronous (Real-Time) Telemedicine: This modality involves a live, two-way interaction between a patient and a healthcare provider. It uses video conferencing, a phone call, or other real-time communication tools to mimic an in-person visit. This is the most common form of telemedicine and is used for virtual doctor’s appointments, follow-up visits, and live consultations.
Asynchronous (“Store-and-Forward”) Telemedicine: This method involves the secure transmission of patient medical information from one location to a healthcare provider at another location for later review. It doesn’t require the patient and provider to be present at the same time. Common examples include a patient sending a dermatologist photos of a skin condition or a primary care physician securely forwarding X-rays and lab results to a radiologist for a remote diagnosis.
Remote Patient Monitoring (RPM): This modality involves the use of digital technology to collect medical and health data from a patient in their home or a remote location. The data is then electronically transmitted to a healthcare provider for review and assessment. RPM is particularly useful for managing chronic conditions like diabetes, hypertension, and heart disease using devices such as continuous glucose monitors, smart scales, or blood pressure cuffs.
Benefits and Key Drivers of Telemedicine
For patients:
- Enhanced Access to Care: Telemedicine dramatically improves access for underserved populations, particularly those residing in remote or rural communities, as well as for individuals with limited mobility, time, or transportation.
- Unmatched Convenience and Time Savings: Virtual visits allow patients to receive care from almost any location, including their home, work, or even a car. This flexibility eliminates the need to travel, take time off from work, or find childcare, leading to significant time and cost savings. In Italy, for example, telehealth services are estimated to save nearly 9.5 hours per year.
- Safety and Reduced Exposure Risk: During periods of high infectious disease transmission, such as the COVID-19 pandemic, telemedicine helps keep both patients and healthcare workers safe.
- Proactive Self-Management: The use of web-based apps, mobile platforms, and wearables empowers patients to take an active role in managing their health. This enables continuous self-monitoring and engagement with their care plan, which has been shown to result in improved health outcomes.
For healthcare providers:
- Increased Efficiency and Productivity: Telemedicine reduces the administrative burden and extensive paperwork traditionally linked to on-site visits through streamlined digital workflows. This allows providers to more efficiently manage scheduling, prescriptions, and charts. One study by the American Medical Association found that healthcare providers who used managed IT services experienced a 27% increase in efficiency, freeing up doctors to dedicate more time to patient care rather than technological issues.
- Cost Reductions and Improved Revenue: Operating a digital practice requires less physical infrastructure, leading to lower overhead expenses for real estate and on-site staff. Furthermore, virtual visits lead to fewer patient no-shows, which reduces associated financial losses and improves the continuity of care. Remote Patient Monitoring (RPM) specifically contributes to increased net patient revenue by improving workflow efficiencies and reducing administrative costs.
- Enhanced Work-Life Balance and Flexibility: For clinicians, telemedicine provides flexible scheduling, allowing them to structure virtual appointments around personal or professional activities. This newfound flexibility can reduce stress and enhance overall professional satisfaction and work-life balance.
For the healthcare system:
- Cost Reduction and Resource Optimization: The ability to provide care remotely significantly reduces the high costs associated with traditional inpatient services. RPM has demonstrated a considerable impact in reducing avoidable emergency department utilization and decreasing unnecessary hospital admissions and readmissions. This allows scarce hospital resources, such as beds and staff, to be reserved for the most acute cases.
- Improved Care Coordination: Technologies like patient portals and virtual consultations among providers improve communication and coordination of care among members of a healthcare team and the patient. These inter-provider virtual consultations can prevent unnecessary referrals to specialists, reduce wait times for patients, and eliminate the need for patients to travel long distances for specialist care.

Major Challenges in the Widespread Adoption
Technological and Infrastructure Hurdles
The fundamental requirement for a successful telehealth visit is a robust technological foundation. A primary barrier is the lack of a connected device with a camera, reliable high-speed internet, and sufficient bandwidth. Even where broadband access is reported, issues of reliability and speed persist, making seamless, real-time video conferencing a challenge.
Human and Behavioral Obstancles
Beyond the technical, the most frequently cited barriers are human-centric, rooted in behavior, perception, and skill sets.
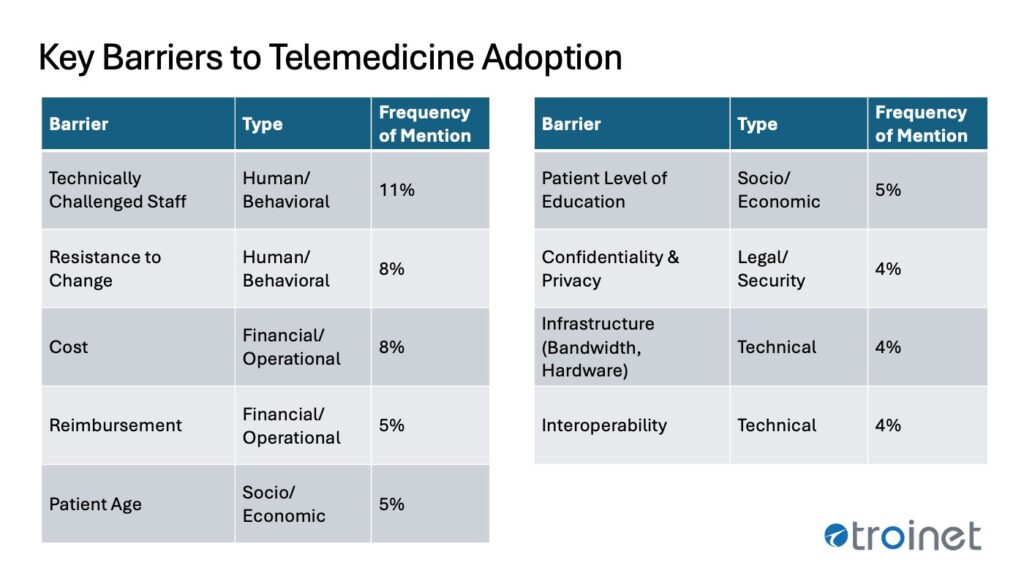
A systematic review found that the top barrier to telemedicine adoption was technically challenged staff, accounting for 11% of all documented occurrences. This highlights a critical need for targeted training and ongoing support.
Following closely behind is resistance to change, a significant obstacle for both providers and patients. This is often tied to clinician perceptions that telemedicine provides impersonal care and a patient preference for traditional, in-person communication. Finally, a lack of simple unawareness of telemedicine’s capabilities, combined with a patient’s age and level of education, each accounted for 5% of the barriers identified.
The Digital Divide: Exacerbating Health Disparities
Data indicates a significant geographic disparity in adoption, with a higher proportion of urban residents having a telehealth visit during the pandemic compared to patients in isolated rural communities (52.8% vs. 41.5%). This is directly tied to the infrastructure hurdles, as rural areas often lack the robust broadband access required for home-based video visits.
Moreover, a clear socioeconomic and demographic divide is present. Emerging data also reveals lower rates of telehealth use among Asian and non-English-speaking patients, and a higher reliance on telephone-only visits among female, Black, and Latinx patients. This suggests that a one-size-fits-all, video-first approach to telemedicine is insufficient and that alternative models, such as clinic-based telehealth hubs in libraries or pharmacies, are needed to ensure equitable access and overcome technological and socioeconomic barriers.
The Strategic Role of Managed Service Providers
The significant benefits and formidable challenges of telemedicine adoption create a clear and critical need for strategic expertise and scalable technical support. It is in this environment that Managed Service Providers (MSPs) have become a modern necessity for the healthcare sector.
1. The MSP Model: A Modern Necessity for Healthcare
A Managed Service Provider is an outsourced third-party company that assumes the ongoing, day-to-day responsibilities, monitoring, and maintenance of a range of tasks and functions for a client organization.
In healthcare, MSPs are primarily contracted to meet the stringent regulatory, operational, and security requirements.
Maintaining an in-house IT team with specialized expertise in healthcare systems and compliance can be prohibitively expensive, especially for smaller hospitals or clinics. MSPs offer a cost-effective alternative, providing access to a team of specialists for a predictable, subscription-based cost. By offloading these burdensome functions, healthcare organizations can reduce overhead, control IT costs, and redirect their focus to their core mission of providing exceptional patient care.
2. MSP as the Backbone of Telemedicine
For telemedicine to function reliably, it requires an IT infrastructure that is always operational, secure, and performant. MSPs provide this essential backbone.
- Ensuring Uptime and Performance: MSPs offer 24/7 system monitoring and proactive maintenance, which significantly reduces the risk of unexpected downtime that could disrupt patient care. They utilize advanced Remote Monitoring and Management (RMM) tools to continuously track the health of a client’s IT infrastructure, identifying vulnerabilities or issues like outdated firmware or limited storage space before they can cause major outages.
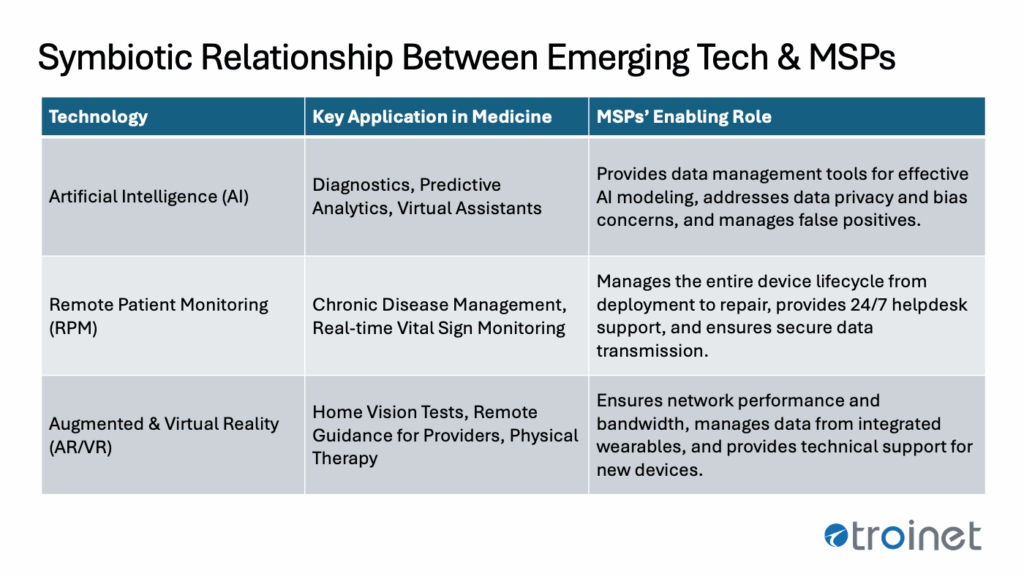
- Specialized Telehealth and RPM Support: MSPs are well-equipped to provide the specific infrastructure support required for a wide range of virtual healthcare services, from secure video consultations to Remote Patient Monitoring. This support can extend to handling the entire device lifecycle for RPM solutions, including staging, kitting, deployment, and ongoing helpdesk support, repairs, and recycling.
3. MSPs Enable and Maintain a Compliant Ecosystem
In an industry where a single data breach can result in significant financial losses, legal penalties, and irreparable damage to patient trust, security is paramount. MSPs provide robust cybersecurity solutions tailored to the unique needs of healthcare.
- HIPAA Compliance: MSPs possess a deep understanding of complex regulations like the Health Insurance Portability and Accountability Act (HIPAA). They ensure that IT systems and data handling practices meet stringent standards through data encryption, secure access controls, and regular security audits.
- Proactive Threat Management: MSPs help enforce essential security measures such as two-factor authentication, strong password policies, and regular patch management to mitigate vulnerabilities and protect sensitive patient data.
Real-World Examples of Successful Telehealth Programs
A review of successful digital care programs highlights the practical application of telemedicine.

For instance, Atrium Health’s innovative Hospital at Home (AH-HaH) program combines in-person visits with virtual consultations and remote patient monitoring kits. This model’s effectiveness hinges on the seamless integration with electronic health records and the reliable functionality of the remote monitoring equipment—all of which are core functions managed by a technology partner.

Ochsner Health’s Connected Maternity Online Monitoring (MOM) program uses digital tools to remotely monitor pregnant patients, reducing the need for in-person visits and improving maternal health outcomes. The success of this program depends on secure data streams and reliable device management, services that are characteristic of an MSP’s offerings.









